Frozen shoulder, also known as adhesive capsulitis, is a disorder characterized by pain, stiffness, and loss of range of motion in the shoulder. It affects about two percent of the general population, and it is most common in women who are over 40 years of age.
Etiology
The causes of frozen shoulder are not fully understood. The process involves thickening and contracture of the shoulder joint capsule. The process does not occur in any other joint in the body. For reasons unkown, the nondominant shoulder is affected more often than the dominant one. Frozen shoulder is not normally associated with calcium deposits, rotator cuff injuries, arthritis or malignancies. The x-rays of the shoulder are completely normal.
Medical problems associated with increased risk of frozen shoulder include diabetes, thyroid disease, Parkinson’s disease, and cardiac disease. Frozen shoulder affects about 10 to 20 percent of people with diabetes, therefore a work-up for diabetes or other disorders may be recommended if a frozen shoulder occurs.
Another risk facter for development of frozen shoulder is prolonged immobilization. After an injury to the shoulder, early motion is usually recommended (assuming that the shoulder is stable) in hopes of avoiding the development of a frozen shoulder.
Diagnosis
This condition is diagnosed by a doctor based on the history of the patient’s symptoms and physical examination. X-rays or MRI (magnetic resonance imaging) studies are sometimes used to rule out other causes of shoulder stiffness and pain, such as rotator cuff tear.
Symptoms
The hallmark of frozen shoulder is pain with restricted motion of the shoulder. The pain is usually dull or aching. It usually becomes worse with motion, and it limits the patient’s use of the affected shoulder and arm. Motion is also limited when someone else attempts to move the shoulder for the patient, as when a doctor performs a physical exam. Some physicians have described the normal course of a frozen shoulder as having three stages. Each stage has been reported to last roughly 4 months, but the time frame for each patient can be highly variable.
- Stage 1: During the “freezing” stage the patient gradually develops a painful shoulder. As the pain worsens, the shoulder loses motion.
- Stage 2: The pain slowly subsides during the “frozen” stage, but the limited range of motion remains.
- Stage 3: During the “thawing” stage the shoulder motion slowly returns toward normal.
Conservative Treatment
Frozen shoulder will generally improve without surgery. The recovery process, however, can be painfully slow (occasionally up to two to three years).
A person with a stiff and painful shoulder should see a physician to ensure that no other injuries or illnesses are present.
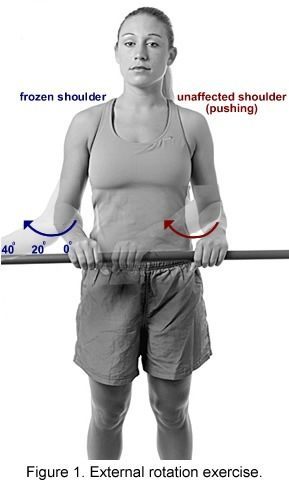
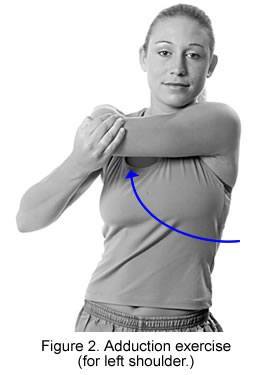
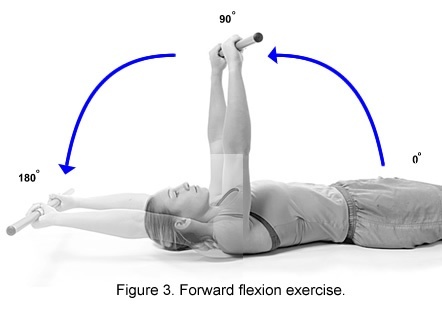
Treatment is focused on pain control and restoration of motion. Pain control can be achieved with anti-inflammatory medications (ibuprofen, naproxen, aspirin, etc.) as well as with injectioned corticosteroids. Physical therapy may help a patient to regain shoulder motion. Stretching or range-of-motion exercises for the shoulder may be done at home or with the assistance of a physical therapist. Example exercises are seen in Figures 1, 2, and 3. A physical therapist can provide additional exercises, as well as other treatments such as massage and heat. If the patient does not respond to these treatments, nerve blocks may be tried to minimize pain and allow for more aggressive physical therapy.
Most patients improve with these simple treatments. However, in some cases the motion does not return completely even after several years. Fortunately, this loss is usually small and does not cause functional limitations.
Surgical Treatment
The vast majority of individuals will get better if given sufficient time, so surgery is not often required. Surgical intervention is considered only after an appropriate course of physical therapy and anti-inflammatory medications has failed.
Surgical intervention is aimed at stretching or releasing the contracted joint capsule of the shoulder. This usually consists of manipulation under anesthesia and/or shoulder arthroscopy:
- Manipulation under anesthesia (Figure 4) involves putting the patient to sleep, then gently and slowly forcing the shoulder to move. This process causes the capsule to stretch, and soft tissue adhesions are broken
- With shoulder arthroscopy, the surgeon makes several small incisions around the shoulder. A small camera (scope) and instruments are inserted through the incisions. The joint capsule is viewed with the scope, and the tight portions of the joint capsule are released
Often, manipulation and arthroscopy are used in combination to obtain a full range of motion for the shoulder joint. Most patients have very good results with these procedures. It is critically important to begin physical therapy immediately after surgery to maintain the motion that was achieved intraoperatively.
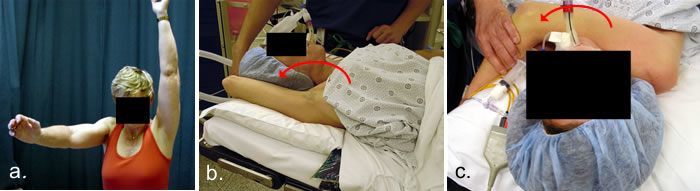
Figure 4.
- This woman was unable to raise her right arm due to adhesive capsulitis. After many months of working with a physical therapist and taking anti-inflammatory medications, she still has a poor range of motion.
- A general anesthetic is administered and the patient is asleep. The arm is then gently taken through a range of motion, which breaks up the adhesions and loosens the shoulder joint. With manipulation she is able to achieve full forward flexion.
- The shoulder is manipulated in another plane (cross-body adduction).




